Slow Metabolism or Is it My Thyroid?
How often have you heard it, or said it yourself …? “My metabolism is ruined and I can’t lose weight no matter how little I eat or how hard I work out”. Do you wake up tired and drag yourself through the day using caffeine and sweets to perk you up? If so, read on and check those that apply:
⬜️ Fatigue…all day long
⬜️ Anxiety/agitation/irritability
⬜️ Insomnia/sleep apnea
⬜️ High cholesterol
⬜️ Irregular or heavy menstrual periods
⬜️ Fertility problems in females
⬜️ Slow heart rate
⬜️ Goiter
⬜️ Poor memory/inability to concentrate
⬜️ Constipation
⬜️ Inability to tolerate cold/cold hands and feet
⬜️ Headaches/migraines
⬜️ Weight gain/inability to lose weight
⬜️ Depression
⬜️ Puffy face/swollen eye lids/fluid retention
⬜️ Muscle and joint pain/Fibromyalgia
⬜️ Hair loss/dry thinning hair/dry skin/brittle nails
⬜️ Miscarriages
This list is just a few of the multiple signs and symptoms of thyroid dysfunction and if you checked most, you may be one of the estimated 20 million Americans with thyroid disease. And, up to 60% of those who do have thyroid disease don’t even know it! If you are female—your risk is eight to nine times that of your male counterpart and about one in every eight women will develop thyroid disease in their lifetime with the peak incidence occurring between ages 30-50 years.
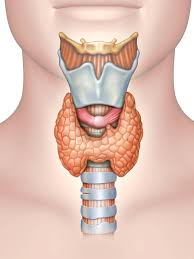
Thyroid disease is one of the most under-diagnosed, mistreated and misunderstood diseases. The small butter-fly shaped gland located in the lower part of your neck affects every cell, tissue and organ in your body. In fact, it is called the “Master of Metabolism” gland. The thyroid gland produces hormones Thyroxine (T4), Triiodothyronine (T3) and Calcitonin. These hormones help with calcium production, bone health and control your metabolism—the conversion of calories and oxygen into energy. This affects critical functions such as energy production, the rate at which your heart beats, the development of a fetus, and affects quality of life.
If you are one of the 60% who has undiagnosed thyroid disease, you likely experience a number of the common symptoms associated with thyroid dysfunction but could also be at higher risk for cardiovascular disease, osteoporosis, infertility, neurologic and muscle-skeletal conditions.
The Many Faces of Thyroid Disease
While hypothyroidism, a deficiency of hormones thyroxine (T4) and triiodothyronine (T3) is the more common thyroid disease, there are many “faces” to thyroid disease.
Hashimoto’s thyroiditis: This is the most common cause of hypothyroidism. This is an immune dysfunction (autoimmune disease) where the immune system develops antibodies that mistakenly “attack and destroy” the gland. Not everyone who has Hashimoto’s disease has low thyroid function but this condition can eventually lead to low hormone production and the need for thyroid replacement medication.
Hyperthyroidism: This is where the gland produces too much thyroxine (T4), or more hormone than the body needs. Symptoms include rapid heart rate (tachycardia); unintentional weight loss; irregular heartbeat (arrhythmia); pounding of your heart (palpitations); nervousness; irritability, anxiety; insomnia; increased appetite; fatigue— (yes fatigue), and increased sweating.
Graves Autoimmune disease: This condition affects about 1 in 200 people and is the most common cause of hyperthyroidism. This is when the immune system mistakenly attacks the gland causing it to produce too much hormone. This condition is commonly triggered by a virus, bacteria or gluten intake.
Thyroid nodules: These are growths on your thyroid gland that may feel like a bump in the middle or on the side of the gland. A goiter (enlarged thyroid gland) can form from many nodules. Nodules can be non-cancerous, become active and produce too much hormone or even cause thyroid cancer.
Thyroid cancer: This is when cells in the gland undergo abnormal changes leading to rapid growth. While thyroid cancer is a scary diagnosis, it is highly treatable and, in most cases, curable.
Testing for Thyroid Disease
In Functional Medicine, we take thyroid testing seriously. We believe since the thyroid gland is the “Master of Metabolism” a very comprehensive approach is warranted.
Laboratory Testing:
These blood tests are used to determine and monitor thyroid disease:
TSH (Thyroid Stimulating Hormone); Total T3; Free T4; Free T3; Reverse T3; Thyroid Peroxidase Antibodies and Thyroglobulin Antibodies –testing for autoimmune disease. (Elevated antibodies can stop thyroid hormones from successfully attaching to receptors, causing symptoms of decreased function even when your blood levels are adequate). Other markers are used if suspecting Graves’ disease.
If test results reveal poor thyroid function, the problem could be associated with certain nutrient deficiencies and testing for these is needed: Urinary Iodine testing, Selenium; Magnesium; Zinc; Vitamin A, B2; B6; B12; Copper; and Iron.
Toxins can affect thyroid function and it may be appropriate to test an array of heavy metals, and environmental toxins.
Adrenal cortisol testing: The adrenal glands and thyroid are intimately connected. Stress can affect enzymes needed for proper thyroid function.
Thyroid ultrasound: These are used to determine the size and shape of the gland and if there are growths present. Ultrasounds can also differentiate between thyroid nodules and cysts. Offered through Kvinna, this is a valuable tool in thyroid testing.
Treatment of Thyroid Disease
Medications:
Thyroid medication is commonly used to regulate thyroid function and there are many options available. Giving T4 (thyroxine) is the “gold standard”. T4 medications include: Levothyroxine, Synthroid, Tirosint, Levoxyl and compounded T4 (made by compounding pharmacies).
T3 medication is often used in conjunction with T4 medication to enhance thyroid function. These medications include Liothyronine, Cytomel, Tirosint and compounded T3 (made by compounding pharmacies).
Natural thyroid medications (from desiccated porcine thyroid gland) include Armour Thyroid, NP thyroid,
Nature-throid, thyroid USP and can also be made through compounding pharmacies. These thyroid preparations include both T4 and T3.
When taking thyroid medications, it is important to have your thyroid labs monitored frequently for optimal thyroid function.
Supplements:
Iodine: This mineral is the main component of thyroxine (T4) and triiodothyronine (T3) and worldwide, the most common cause of low thyroid function and often the cause of a goiter. Too much iodine can cause hyperthyroidism so it is important to monitor labs.
Testing and treating nutrients specific for thyroid function is crucial. Often, adding key nutrients is enough to optimize thyroid function.
Diet:
Taming the blood sugar beast: Thyroid function is intimately related to blood sugar control. Low thyroid function slows down the absorption of glucose causing symptoms of hypoglycemia. This activates the adrenal glands to raise blood sugar, but to no avail. It is critically important to control blood sugar through your diet. Adequate lean, high-quality protein which includes shell fish (Iodine), moderate fibrous, crispy carbs (I call these “rabbit food veggies”) and healthy fats, ample water (1/2 your body weight in ounces).
Inadequate protein, high carbohydrate diets and excessive alcohol intake adversely affect enzymes needed for thyroid function and conversion of nutrients into energy.
A significant number of people who have autoimmune thyroid disease also have Celiac disease or a gluten immune sensitivity which may be contributing to the destruction of the gland. Gluten is a protein component in grains such as spelt, wheat, rye, and barley. Experts say that a gluten-free diet could at least stop the destruction if this is the cause of a person’s autoimmune disorder.
Being a Functional Medicine nurse practitioner and having suffered from autoimmune hypothyroid disease myself, I fully understand the importance, yet difficulty, of following a gluten-free diet, making sure I am controlling my blood sugar via diet, modulating stress and getting the proper nutrients I need.
It takes time, commitment, and dedication to being healthy and there is no better time than NOW to make that commitment.
Author: Debbie Judd ARNP
Owner, The Metabolic Institute

American Thyroid Association. General Information/Press Room. (https://www.thyroid.org/media-main/press-room/) Accessed 03/18/2022.
National Library of Medicine. Hashimoto’s thyroiditis following Graves’ disease. (https://pubmed.ncbi.nlm.nih.gov/20305330/) Accessed 03/13/2022.
US Department of Health & Human Services, Office of Women’s Health. Thyroid disease. (https://www.womenshealth.gov/a-z-topics/thyroid-disease) Accessed 03/18/2022.
MedlinePlus [Internet]. Bethesda (MD): National Library of Medicine (US); [updated on 16 March 2022; cited 17 March 2022] Available from: https://medlineplus.gov/hypothyroidism.
US Department of Health and Human Services, National Institute of Diabetes and Digestive and Kidney Diseases. Hyperthyroidism (Overactive Thyroid). (https://www.niddk.nih.gov/health-information/endocrine-diseases/hyperthyroidism?dkrd=hispt0298) Accessed 03/17/2022.



Leave A Comment
You must be logged in to post a comment.